COVID-19 Testing & Care
COVID-19 Pruebas y cuidados
Protect yourself and others. Choose to get vaccinated, wear a mask in indoor public spaces and wash hands often.
COVID-19 Testing Overview:
(click on each box to expand for details)
COVID-19 Viral Testing (rapid and PCR) is available at:
- Tillamook County Community Health Center
- Appointments required, please call 503-842-3900
- Adventist Health – all medical offices (Estacada, Lincoln City, Manzanita, Pacific City, Sheridan, Tillamook, Vernonia, and Welches).
- For Tillamook locations, call 503-842-5546
- See website for details.
- Rinehart Clinic
- Appointments required, please call 1-800-368-5182
- See website for details.
Two kinds of tests are available for COVID-19: viral tests and antibody tests.
- A viral test tells you if you have a current infection.
- An antibody test might tell you if you had a past infection.
At the health center, we offer the viral test only done by a nasal swab. We have two types of viral nasal swab test: rapid/quick-test and PCR. The rapid test provides results in 15 minutes. The PCR test requires the swab to be sent to a lab for processing, results can take 3-4 days. Both nasal swab tests require the swab to be placed just inside the nostril, no further up. The swab takes seconds to complete.
A viral test for COVID-19 tells you if you have a current infection. During a viral test, the inside of the nose is swabbed, and the swab is then used to detect the presence of COVID-19 using a quick-antigen test or sending the swab to a lab to be processed (PCR-test).
- Quick-Antigen test (Rapid Test): Available via home/self-kits or from healthcare facilities. Follow the manufacture instructions included with the kit if performing at home. Results are typically available within 15 minutes. This test can only detect a higher presence of the virus in your body and is often recommended to use when symptomatic or 3-5 days after a potential exposure.
- PCR test: Available via home/self-kits or from healthcare facilities. Follow the manufacture instructions included with the kit if performing at home. These tests require the sample to be sent to a lab facility for processing. Results are typically available within 2-3 days. This test can detect lower levels of the virus in the body due to the more advanced equipment used in the lab facility. Recommended for use for asymptomatic close contacts and for those with symptoms after a negative quick-antigen test.
The federal site to order free quick (rapid) antigen home COVID-19 test, up to 4 per U.S. household is now live: https://www.covidtests.gov/
Self-tests (also known as home-tests) may be used if you have COVID-19 symptoms or have been exposed or potentially exposed to an individual with COVID-19.
Even if you don’t have symptoms and have not been exposed to an individual with COVID-19, using a self-test before gathering indoors with others can give you information about the risk of spreading the virus that causes COVID-19.
Self-tests can be purchased online or in pharmacies and retail stores. Home-test kits may be a covered benefit, please contact your health insurance. Visit FDA’s website for a list of authorized tests. Some self-tests may have age limitations.
U.S. Households can now order up to four COVID-19 home test kits for free using the new federal site: live: https://www.covidtests.gov/
Super easy and quick to fill out- the tests will ship out late January.
Need help? Contact OHA COVID-19 Support Hotline: 866-917-8881 or 211
Up to four COVID-19 home tests per month are covered by Oregon Health Plan (OHP) for OHP members when purchased in store (not online) from a pharmacy. Learn more here.
Read the complete manufacturer’s instructions for use before using the test. Talk to a healthcare provider if you have questions about the test or your results. Refer to CDC’s videos on How to Use a Self-Test and How to Interpret Self-Test Results.
You should isolate if you test positive. For early treatment options, contact your healthcare provider right away after a positive test result.
Please refer to your employer for questions regarding work and self-test results. If a note for work is required by an employer, employees must repeat testing in a healthcare setting for a provider to verify test results and provide work note.
COVID-19 testing is available at:
- Tillamook County Community Health Center
- Appointments required, please call 503-842-3900
- Tillamook County public health has a small supply of COVID-19 home tests for communities most at risk of COVID-19 and disproportionately impacted, learn more here
- Adventist Health – all medical offices (Estacada, Lincoln City, Manzanita, Pacific City, Sheridan, Tillamook, Vernonia, and Welches).
- See website for details.
- A limited amount of self-tests will be available from Adventist Health at all medical offices (Estacada, Lincoln City, Manzanita, Pacific City, Sheridan, Tillamook, Vernonia, and Welches) by walk-in or scheduled appointment as soon as the kits are delivered. Expected early January. Contact Adventist Health for more information (503) 842-4444.
- Rinehart Clinic
- Appointments required, please call 1-800-368-5182
- See website for details.
COVID-19 viral tests (nasal swab) detect the presence of the virus in your body (including all variants). The viral test itself cannot tell you which variant you have, just that you do have the virus or not (positive or negative).
There is no specific viral test for the Omicron variant, or for other variants.
Once the viral tests are performed, the collected samples/ swabs are then sent out to laboratories for scientist to perform analysis on the swab including the PCR test and genetic sequencing on a subset of viral tests that are positive, looking for the specific mutations that appear in specific variants.
- Genetic Sequencing is a process in which scientists map the entire genetic makeup of a virus. This allows them to determine which variants are circulating in a certain area and how prevalent they are.
There is very specific guidance available on Oregon Health Authority’s COVID-19 information page that must be met in order for sequencing to be performed.
With limited labs that can perform this special analysis and county public health’s going to the Oregon State Public Health Lab it is unfortunately not something we can have done on every test, or even majority, so many tests do not get sequenced.
The variant type does not change the diagnosis, care options, or isolation guidance. The information when available is helpful to better understand and anticipate disease spread for public health and healthcare providers.
COVID-19 variant tracking data is available from Oregon Health Authority, here
Wastewater surveillance has been successfully used as a method for early detection diseases at the community level and has been previously used in Oregon for identifying emerging variants, including Delta. This method of disease surveillance can generate data trends that are helpful for informing on the total disease burden in a community, but is not used to measure the number of infected individuals so this surveillance often used in addition to other surveillance tools, such as genetic sequencing of viral COVID-19 tests.
SARS-CoV-2, the virus that causes COVID-19 can be shed in the feces of individuals with symptomatic or asymptomatic infection; therefore, wastewater surveillance can capture data on both types of infection. While SARS-CoV-2 can be shed in the feces of individuals with COVID-19, from the CDC, there is no information to date that anyone has become sick with COVID-19 because of direct exposure to treated or untreated wastewater
Learn more from the CDC, here
Who Should Get Tested?
(click on each box to expand for details)
If you have symptoms of COVID-19 you should get tested regardless of your vaccination status.
From the CDC, people with COVID-19 have had a wide range of symptoms reported – ranging from mild symptoms to severe illness. Symptoms may appear 2-14 days after exposure to the virus. Anyone can have mild to severe symptoms. People with these symptoms may have COVID-19:
- Fever or chills
- Cough
- Shortness of breath or difficulty breathing
- Fatigue
- Muscle or body aches
- Headache
- New loss of taste or smell
- Sore throat
- Congestion or runny nose
- Nausea or vomiting
- Diarrhea
This list does not include all possible symptoms. CDC will continue to update this list as we learn more about COVID-19. Older adults and people who have severe underlying medical conditions like heart or lung disease or diabetes seem to be at higher risk for developing more serious complications from COVID-19 illness.
When to Seek Emergency Medical Attention
Look for emergency warning signs* for COVID-19. If someone is showing any of these signs, seek emergency medical care immediately:
- Trouble breathing
- Persistent pain or pressure in the chest
- New confusion
- Inability to wake or stay awake
- Pale, gray, or blue-colored skin, lips, or nail beds, depending on skin tone
*This list is not all possible symptoms. Please call your medical provider for any other symptoms that are severe or concerning to you.
Call 911 or call ahead to your local emergency facility: Notify the operator that you are seeking care for someone who has or may have COVID-19.
If you have been in close contact with someone with COVID-19, you should be tested regardless of your vaccination status. Close contact means being within 6 feet of someone for 15 minutes or more over the course of a day, with or without a mask or face shield.
If you are being tested because you have been in close contact with someone who has COVID-19, it is best to wait three days after you have been together before being tested. The test is less accurate if you test too early. You should stay home and away from others while you wait.
What to do After a Positive Test Result?
Please report any positive test result as soon as possible using this survey link, to start the case investigation and support process. Need help? Call 866‑917‑8881
(click on each box to expand for details)
Please report any positive test result as soon as possible using this survey link, to start the case investigation and support process. Need help? Call 866‑917‑8881
Isolation is used to separate people infected with COVID-19 from those who are not infected.
People who are in isolation should stay home until it’s safe for them to be around others. At home, anyone sick or infected should separate from others, stay in a specific “sick room” or area, and use a separate bathroom (if available).
How Long to Isolate – General Public
Isolation: people (including K-12 settings) who have tested positive for COVID-19 with no symptoms or are showing mild to moderate symptoms of COVID-19 should isolate regardless of vaccination status.
- Start isolation for 5 full days.
- Individuals can end isolation after 5 full days since symptom onset if they are fever-free for 24 hours without the use of fever-reducing medication and their other symptoms have improved.
- Day 0 is the day symptoms began or the day the person took a test that had a positive result. Day 1 is the day after symptoms began or, if a person does not have symptoms, the day after the person tested positive (use the date the test was collected).
- If they continue to have fever or their other symptoms have not improved after 5 days of isolation, they should stay in isolation until they are fever-free for 24 hours without the use of fever-reducing medication and their other symptoms have improved.
- Individuals should continue to wear a well-fitting mask around others at home and in public places for an additional 5 days (day 6 through day 10) after the end of their 5-day isolation.
People regardless of vaccination status with severe to critical illness, including those who were hospitalized for their COVID-19 illness, or who are severely immunocompromised, the minimum period of isolation is 20 days. That is, these cases should isolate until at least 20 days since symptom onset or first positive test, whichever is earlier, and they have been fever free without the use of fever-reducing medications with other symptoms resolving for at least 24 hours.
Subject to change. For further details visit the Center for Disease Control and Prevention Quarantine and Isolation webpage.
What to do
- Monitor your symptoms. If you have an emergency warning sign (including trouble breathing), seek emergency medical care immediately.
- Stay in a separate room from other household members, if possible.
- Use a separate bathroom, if possible.
- Avoid contact with other members of the household and pets.
- Don’t share personal household items, like cups, towels, and utensils.
- Wear a mask when around other people if able.
Learn more about what to do if you are sick and how to notify your contacts.
Use the CDC Quarantine and Isolation Calculator tool to help determine how long you need to isolate, quarantine, or take other steps to prevent spreading COVID-19.
Information from the CDC, see more here
Please report any positive test result as soon as possible using this survey link, to start the case investigation and support process. Need help? Call 866‑917‑8881
Isolation is used to separate people infected with COVID-19 from those who are not infected.
People who are in isolation should stay home until it’s safe for them to be around others. At home, anyone sick or infected should separate from others, stay in a specific “sick room” or area, and use a separate bathroom (if available).
How Long to Isolate – Healthcare Workers
Isolation: healthcare workers who have presumed or confirmed COVID-19 or are showing symptoms of COVID-19 should isolate regardless of vaccination status.
- Start isolation for 10 full days.
- Individuals may end isolation after 7 full days since symptom onset if they are fever-free for 24 hours without the use of fever-reducing medication and their other symptoms have improved AND they are retested between day 5 to 7 of isolation for COVID-19 and test negative.
- Day 0 is the day symptoms began or the day the person took a test that had a positive result. Day 1 is the day after symptoms began or, if a person does not have symptoms, the day after the person tested positive (use the date the test was collected).
- If they continue to have fever or their other symptoms have not improved, or they test positive on retest or are unable to get tested after 7 days of isolation, they should stay in isolation for a total of 10 full days from onset of symptoms or original test date. In addition, must be fever-free for 24 hours without the use of fever-reducing medication and their other symptoms have improved for isolation to end after 10 days.
People regardless of vaccination status with severe to critical illness, including those who were hospitalized for their COVID-19 illness, or who are severely immunocompromised, the minimum period of isolation is 20 days. That is, these cases should isolate until at least 20 days since symptom onset or first positive test, whichever is earlier, and they have been fever free without the use of fever-reducing medications with other symptoms resolving for at least 24 hours.
Subject to change. For further details see Oregon Health Authority’s Interim Guidance for Managing Healthcare Personnel with SARSCoV-2 Infection or Exposure.
What to do
- Monitor your symptoms. If you have an emergency warning sign (including trouble breathing), seek emergency medical care immediately.
- Stay in a separate room from other household members, if possible.
- Use a separate bathroom, if possible.
- Avoid contact with other members of the household and pets.
- Don’t share personal household items, like cups, towels, and utensils.
- Wear a mask when around other people if able.
Learn more about what to do if you are sick and how to notify your contacts.
Information from the CDC, see more here
What to do After an Exposure to COVID-19/ Close Contact?
(click on each box to expand for details)
Quarantine is used to separate and restricts the movement of people who were exposed to a contagious disease to see if they become sick after close contact (within 6 feet of someone for a cumulative total of 15 minutes or more over a 24-hour period) with someone who has COVID-19.
Effective March 12, quarantine will no longer be recommended for people within the general population who have been exposed to someone who has COVID-19, regardless of vaccination status. This includes children and staff in K-12 and childcare settings.
All are recommended to:
- Consider wearing a well-fitting mask for 10 days after exposure.
- Watch for symptoms until 10 days after exposure.
- If you have symptoms, immediately self-isolate and contact your local public health authority or healthcare provider.
Information from the CDC, see more here
Quarantine is used to separate and restricts the movement of people who were exposed to a contagious disease to see if they become sick after close contact (within 6 feet of someone for a cumulative total of 15 minutes or more over a 24-hour period) with someone who has COVID-19.
How Long to Quarantine – Healthcare Workers
Quarantine: Healthcare workers in higher risk settings who come into close contact with someone with COVID-19 quarantine length depends upon vaccination status.
Those up to date on COVID-19 vaccination as defined by CDC (see definition below) AND individuals who had confirmed COVID-19 (tested positive using a COVID-19 viral test) within the last 90 days:
- Get tested on day 2 after having close contact with someone with COVID-19. If they test positive or develop COVID-19 symptoms, they should follow recommendations for isolation.
- If they test negative, no quarantine required.
- Wear a well-fitting mask around others for 10 days from the date of their last close contact with someone with COVID-19 (the date of last close contact is considered day 0) and watch for symptoms of COVID-19.
- Get retested between day 5 to 7 after having close contact with someone with COVID-19. If they test positive or develop COVID-19 symptoms, they should follow recommendations for isolation.
Those NOT up to date on COVID-19 vaccination as defined by CDC (see definition below):
- Quarantine for at least 10 days after their last close contact with someone with COVID-19. Day 0 is the last day you had close contact with the infected individual.
- Individuals in quarantine should not go to work or other in-person events/activities.
- May get tested between day 5 to 7 of quarantine and if the test is negative may return to work after 7 days of quarantine. Wear a well-fitting mask around others for 10 days from the date of their last close contact with someone with COVID-19 (the date of last close contact is considered day 0) and watch for symptoms of COVID-19.
- Get retested between day 5 thru 7 after having close contact with someone with COVID-19. If they test positive or develop COVID-19 symptoms, they should follow recommendations for isolation.
- If unable to get tested between day 5 and 7 of quarantine, healthcare worker should continue quarantine for the 10-day period. After 10 days, quarantine may end, and healthcare worker may return to work.
Subject to change. For further details see Oregon Health Authority’s Interim Guidance for Managing Healthcare Personnel with SARSCoV-2 Infection or Exposure.
vaccination status Up to Date definition:
-
Boosted,
-
or completed the primary series of Pfizer or Moderna within the last 6 months,
-
or completed the primary series of J&J within the last 2 months.
vaccination status NOT Up to Date definition:
-
unvaccinated,
-
or has not completed the primary series of any COVID-19 vaccine,
-
or completed the primary series of Pfizer or Moderna over 6 months ago and is not boosted,
-
or completed the primary series of J&J over 2 months ago and is not boosted.
What to do
- Follow the quarantine timeframe depending on COVID-19 vaccine status.
- Watch for fever (100.4◦F), cough, shortness of breath, or other symptoms of COVID-19.
- If possible, stay away from people you live with, especially people who are at higher risk for getting very sick from COVID-19.
After quarantine
- Watch for symptoms until 10 days after exposure.
- If you have symptoms, immediately self-isolate and contact your local public health authority or healthcare provider.
Use the CDC Quarantine and Isolation Calculator tool to help determine how long you need to isolate, quarantine, or take other steps to prevent spreading COVID-19.
Information from the CDC, see more here
Treatment & Community Resources
(click on each box to expand for details)
There are more treatment options now available in the battle against coronavirus disease. Talk to your health care provider about available treatment options if you have COVID-19 as soon as possible, some treatment options need to be started as early as 5 days from your positive test date.
Your provider will know the best option for you, based on your symptoms, risks, and health history.
What treatments are available for COVID-19?
The best way to fight COVID-19 is to avoid getting it in the first place. That means wearing a well-fitting mask, keeping gatherings small and outdoors if possible and getting vaccinated (including a booster dose if eligible.)
But the virus is still spreading widely, so even if you do follow every safety protocol you still might become infected, and potentially severely ill.

Although most cases of COVID-19 don’t require hospitalization, some people have conditions that increase their risk of severe infection, such as asthma, diabetes, or heart disease. They may also be on medications that weaken their immune systems or have a chronic illness that might worsen the effects of COVID-19. The CDC has a comprehensive list of certain medical conditions that make someone higher risk.
For these people, there are several COVID-19 treatments available:
Oral Antiviral treatments from Pfizer, Merck
The FDA recently approved two oral antiviral medications that dramatically reduce the chances of hospitalization, but they must be administered as soon as possible after a positive COVID-19 diagnosis and within the first five days of symptoms to be effective.
- Paxlovid (from Pfizer) works by disrupting the virus’s ability to mutate. It specifically targets an enzyme that helps certain viral proteins form correctly.
- Molnupiravir (from Merck) works by introducing mutations directly into the virus’s genetic makeup. As the virus copies itself, it gets so mutated that it can no longer function. There are some safety concerns because it alters the virus’s genetic information. Some experts worry about adverse effects, especially in pregnant people and in children.
Because of nationwide shortages, neither of these medications is widely available. Do not go to the emergency room seeking these medications if you don’t require emergency care. If you’re experiencing symptoms, check with your regular doctor if you have one, or visit an urgent care clinic or call Adventist pharmacy at 503-815-2341 to speak to a pharmacist.
Consider establishing care with a provider using the following contacts: Tillamook County Community Health Center (503-842-3900), Adventist Health Tillamook (503-842-5546) or Rinehart Clinic (1-800-368-5182).
Remdesivir
The antiviral drug remdesivir also acts on the virus’ genetic material, blocking its ability to mutate. Remdesivir (also known as its brand name, Veklury) was first approved in October 2020 for COVID-19 patients ages 12 and older requiring hospitalization. On January 21, 2022, the FDA amended its approval to include COVID-19 patients ages 12 and older who do not require hospitalization but are at risk for severe disease. Additionally, the FDA has authorized remdesivir for pediatric patients younger than 12 years old, weighing at least 3.5 kg (about 7 pounds).
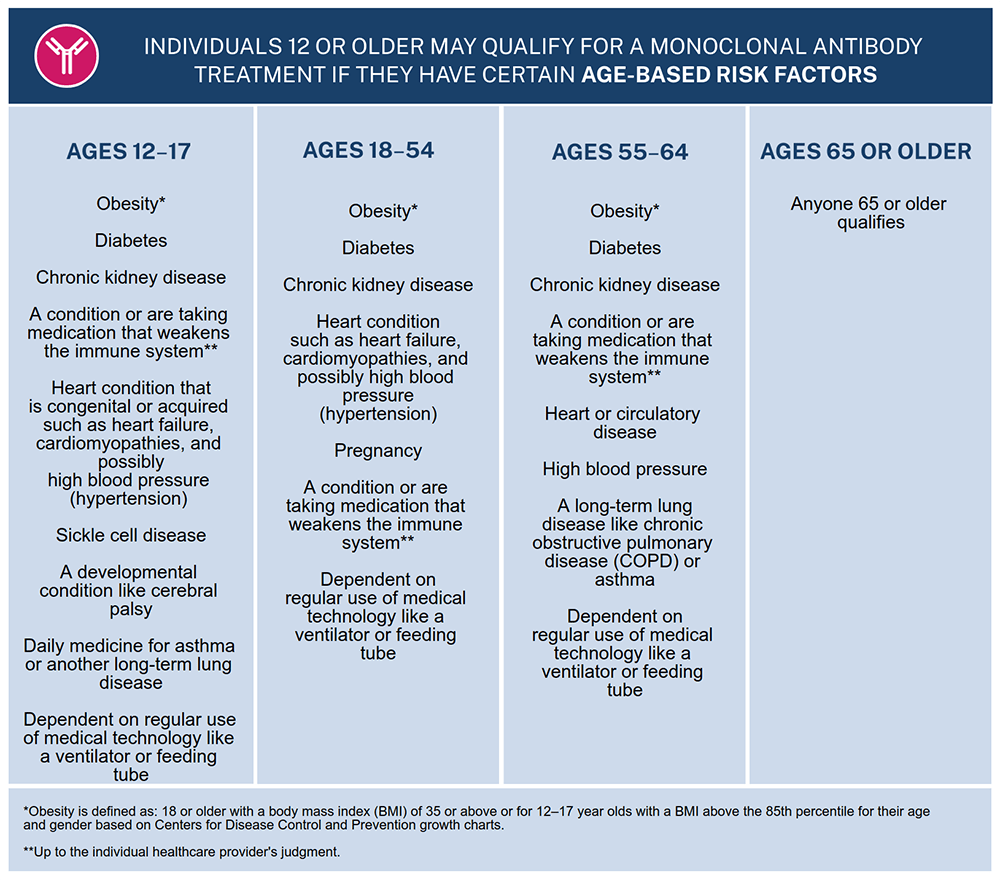
Monoclonal Antibodies
Monoclonal antibodies work by mimicking one of your body’s immune responses. When your immune system detects a foreign invader like a virus, it unleashes antibodies. Those antibodies latch onto the virus, telling your immune system which cells to destroy.
Monoclonal antibodies are created in a lab and are administered via injection directly into the bloodstream, or into an arm or other area on the body like a shot.
There are several currently authorized monoclonal antibody treatments available in the U.S., and they each work slightly differently. However, only one, called Sotrovimabv, seems to be effective against the Omicron variant.
Only certain people can receive monoclonal antibodies. See the chart below for eligibility guidelines.
(Chart from: https://combatcovid.hhs.gov/i-have-covid-19/how-do-i-know-if-im-high-risk and content in this section from https://covidblog.oregon.gov/what-kind-of-treatments-exist-for-covid-19/)
The FDA continues to work with developers, researchers, manufacturers, the National Institutes of Health, and other partners to help expedite the development and availability of therapeutic drugs and biological products to prevent or treat COVID-19. To check whether a drug is approved by FDA, search the database of approved drugs by visiting the Drugs@FDA database.
What should I do if I have, or think I have, COVID-19?
The Centers for Disease Control and Prevention have recommendations for people who are sick with COVID-19 or think they might have COVID-19.
In general, most people have mild illness and can recover at home. If you think you have been exposed to COVID-19, notify your doctor, monitor your symptoms, and get emergency medical care immediately for emergency warning signs, such as trouble breathing.
If you think you have COVID-19 and need a test, contact your health care provider, local health department, or call 211 to find a community testing site.
This information is from the U.S. Food & Drug Administration page
How can I access these treatments?
Depending on your medical history, risks, and symptoms, your health care provider can help you determine whether a therapy that is FDA-approved, or available under an EUA, is right for you.
The following websites contain information regarding access to monoclonal antibody treatments for COVID-19:
This information is from the U.S. Food & Drug Administration page
What if my health care provider doesn’t know about these treatment options?
Information about treatment options is available on the COVID-19 Frequently Asked Questions web page.
For information specifically about EUAs, direct your health care provider to the FDA’s Emergency Use Authorization (EUA) page, where fact sheets for health care providers are available on authorized treatments. Your health care provider can also contact our Division of Drug Information at 301-796-3400 or druginfo@fda.hhs.gov.
This information is from the U.S. Food & Drug Administration page
Staying home until you can no longer spread the virus is important but staying home may not be easy. If you need assistance, there are options to support you.
If you need help finding a place to isolate or quarantine, call Tillamook County Community Health Center at: 503-842-3924.
If you need assistance with food, grocery or medication delivery, call the YMCA Care line at: 503-374-0750.
If you would like to talk with someone on the difficult emotions you may be feeling, please know that you are not alone. Trained professionals are waiting for your call or text:
-
- Tillamook Family Counseling Center: (503) 842-8201 or 1-800-962-2851.
- Tides of Change: 503-842-9486
- National Suicide Prevention Lifeline – 800-273 TALK(8255); www.suicidepreventionlifeline.org
- Oregon Senior Peer Outreach: 1800-736-4676
- SAMHSA Disaster Distress Hotline: 1800-985-5990
- Senior Loneliness Line: 503- 200-1633
- The Friendship Line – 1800-971-001
- Dual Diagnosis Anonymous: online meeting schedule
- Helping Children Cope – online resource
- National Alliance for Mentally Ill (NAMI)- www.namiwash.org
Definitions
(click on each box to expand for details)
- Boosted,
- or completed the primary series of Pfizer or
Moderna within the last 6 months, - or completed the primary series of J&J within
the last 2 months.
- Unvaccinated,
- or has not completed the primary series of any COVID-19 vaccine
- or completed the primary series of Pfizer or Moderna over 6 months ago and is not boosted,
- or completed the primary series of J&J over 2 months ago and is not boosted.
Introducing our COVID-19 Acute Care Clinic
COVID-19 testing and care is available for individuals experiencing symptoms or who have had close contact with a confirmed COVID-19 case at our acute care clinic located at 2111 8th St. Tillamook.
Hours:
Monday – Friday
8am – 12pm
Appointments are required, please call: 503-842-3900
Protégete a ti mismo y a los demás. Opte por vacunarse, usar mascarilla en espacios públicos cerrados y lavarse las manos con frecuencia.
la traducción al español se añadirá tan pronto como esté disponible
Pruebas de detección del COVID-19: visión general:
(haga clic en cada casilla para ampliar los detalles)
La prueba viral COVID-19 (rápida y PCR) está disponible en:
- Centro de Salud Comunitaria del Condado de Tillamook
- Se requiere una cita, por favor llame al 503-842-3900
- Adventist Health – todos los consultorios médicos (Estacada,
- Lincoln City, Manzanita, Pacific City, Sheridan, Tillamook, Vernonia y Welches).
- Para los consultorios de Tillamook, llame al 503-842-5546
- Consulte el sitio web para obtener más detalles.
- Clínica Rinehart
- Se requiere una cita, por favor llame al 1-800-368-5182
Vea el sitio web para más detalles.
- Se requiere una cita, por favor llame al 1-800-368-5182
Hay dos tipos de pruebas de detección del COVID-19 disponibles: pruebas virales y pruebas de anticuerpos.
- Una prueba viral indica si actualmente tiene una infección.
- Una prueba de anticuerpos podría indicar si anteriormente tuvo una infección.
En el centro de salud, ofrecemos la prueba vírica sólo mediante un hisopo nasal. Tenemos dos tipos de pruebas virales con hisopo nasal: la rápida y la PCR. La prueba rápida proporciona resultados en 15 minutos. La prueba PCR requiere que el hisopo se envíe a un laboratorio para su procesamiento, los resultados pueden tardar 3-4 días. Ambas pruebas de hisopo nasal requieren que el hisopo se coloque justo dentro de la fosa nasal, no más arriba. El hisopo tarda segundos en completarse.
Una prueba viral para COVID-19 le indica si tiene una infección actual. Durante una prueba viral, se toma un hisopo del interior de la nariz, y el hisopo se utiliza para detectar la presencia de COVID-19 utilizando una prueba de antígeno rápido o enviando el hisopo a un laboratorio para ser procesado (prueba PCR).
- Prueba de antígeno rápido (Rapid Test): Disponible a través de kits caseros/autocomprobantes o en centros sanitarios. Siga las instrucciones de fabricación incluidas en el kit si lo realiza en casa. Los resultados suelen estar disponibles en 15 minutos. Esta prueba sólo puede detectar una mayor presencia del virus en el organismo y suele recomendarse su uso cuando se presentan síntomas o entre 3 y 5 días después de una posible exposición.
- Prueba PCR: Disponible a través de kits caseros/autoconvocados o en centros sanitarios. Siga las instrucciones de fabricación incluidas en el kit si lo realiza en casa. Estas pruebas requieren el envío de la muestra a un laboratorio para su procesamiento. Los resultados suelen estar disponibles en 2-3 días. Esta prueba puede detectar niveles más bajos del virus en el cuerpo debido al equipo más avanzado que se utiliza en el laboratorio. Se recomienda su uso para contactos cercanos asintomáticos y para aquellos con síntomas después de una prueba de antígeno rápido negativa.
El sitio federal para pedir gratuitamente la prueba casera de antígeno rápido COVID-19, hasta 4 por hogar en EE.UU. ya está en funcionamiento: https://www.covidtests.gov/
Las pruebas caseras pueden usarse si presenta síntomas de COVID-19 o ha estado expuesto o posiblemente expuesto a una persona con COVID-19.
Incluso si no presenta síntomas y no ha estado expuesto a una persona con COVID-19, hacerse una prueba casera antes de participar en encuentros en espacios cerrados con otras personas puede brindarle información acerca del riesgo de propagar el virus que causa el COVID-19.
Las autopruebas pueden adquirirse en línea o en farmacias y tiendas minoristas. Los kits de pruebas caseras pueden ser un beneficio cubierto, por favor, póngase en contacto con su seguro de salud. Visite el sitio web de la FDA para ver una lista de las pruebas de detección autorizadas. Algunas autopruebas pueden tener limitaciones de edad.
Los hogares de EE.UU. ya pueden solicitar gratuitamente hasta cuatro kits de pruebas domésticas COVID-19 a través del nuevo sitio federal: live: https://www.covidtests.gov/
Es muy fácil y rápido de rellenar. Las pruebas se enviarán a finales de enero.
¿Necesita ayuda? Póngase en contacto con la línea directa de apoyo a COVID-19 de la OHA: 866-917-8881 o 211
El Plan de Salud de Oregón (OHP) cubre hasta cuatro pruebas caseras COVID-19 al mes para los miembros del OHP cuando se compran en la tienda (no en línea) de una farmacia. Obtenga más información aquí.
Lea todas las instrucciones de uso del fabricante antes de hacerse la prueba de detección. Si tiene dudas acerca de la prueba o sus resultados, hable con un proveedor de atención médica. Vea los videos de los CDC sobre Cómo usar una prueba casera y Cómo interpretar los resultados de una prueba de detección casera. Debe aislarse si el resultado de su prueba de detección es positivo.
Las pruebas de COVID-19 están disponibles en:
- Centro de Salud Comunitario del Condado de Tillamook
- Se requiere una cita, por favor llame al 503-842-3900
- La sanidad pública del condado de Tillamook dispone de un pequeño suministro de pruebas caseras de COVID-19 para las comunidades más expuestas al riesgo de COVID-19 y desproporcionadamente afectadas, obtenga más información aquí
- Adventist Health – todos los consultorios médicos (Estacada, Lincoln City, Manzanita, Pacific City, Sheridan, Tillamook, Vernonia y Welches).
- Consulte el sitio web para obtener más detalles.
Una cantidad limitada de autopruebas estará disponible en Adventist Health en todos los consultorios médicos (Estacada, Lincoln City, Manzanita, Pacific City, Sheridan, Tillamook, Vernonia y Welches) sin cita previa o con cita programada tan pronto como se entreguen los kits. Se espera a principios de enero. - Póngase en contacto con Adventist Health para obtener más información (503) 842-4444.
- Consulte el sitio web para obtener más detalles.
- Clínica Rinehart
- Se requiere cita, por favor llame al 1-800-368-5182
- Vea el sitio web para más detalles.
Las pruebas virales COVID-19 (hisopo nasal) detectan la presencia del virus en su cuerpo (incluyendo todas las variantes). La prueba vírica en sí no puede decir qué variante tiene, sólo que tiene el virus o no (positivo o negativo).
No existe una prueba vírica específica para la variante Omicron, ni para otras variantes.
Una vez realizadas las pruebas víricas, las muestras recogidas/los hisopos se envían a los laboratorios para que los científicos realicen el análisis del hisopo, incluida la prueba PCR y la secuenciación genética en un subconjunto de pruebas víricas que son positivas, buscando las mutaciones específicas que aparecen en variantes concretas.
La secuenciación genética es un proceso en el que los científicos mapean toda la composición genética de un virus. Esto les permite determinar qué variantes circulan en una zona determinada y su prevalencia.
Hay una guía muy específica disponible en la página de información COVID-19 de la Autoridad Sanitaria de Oregón que debe cumplirse para que se realice la secuenciación.
Con los limitados laboratorios que pueden realizar este análisis especial y la salud pública del condado que va al Laboratorio de Salud Pública del Estado de Oregón, lamentablemente no es algo que podamos hacer en todas las pruebas, o incluso en la mayoría, por lo que muchas pruebas no se secuencian.
El tipo de variante no cambia el diagnóstico, las opciones de atención o la orientación sobre el aislamiento. La información, cuando está disponible, es útil para comprender mejor y anticipar la propagación de la enfermedad para la salud pública y los proveedores de atención médica.
Los datos de seguimiento de las variantes de COVID-19 están disponibles aquí
La vigilancia de las aguas residuales se ha utilizado con éxito como método de detección precoz de enfermedades a nivel comunitario y se ha utilizado anteriormente en Oregón para identificar variantes emergentes, incluida la delta. Este método de vigilancia de la enfermedad puede generar tendencias de datos que son útiles para informar sobre la carga total de la enfermedad en una comunidad, pero no se utiliza para medir el número de individuos infectados, por lo que esta vigilancia se utiliza a menudo además de otras herramientas de vigilancia, como la secuenciación genética de las pruebas de COVID-19 viral.
El SARS-CoV-2, el virus que causa el COVID-19, puede eliminarse en las heces de los individuos con infección sintomática o asintomática; por lo tanto, la vigilancia de las aguas residuales puede captar datos sobre ambos tipos de infección. Si bien el SARS-CoV-2 puede eliminarse en las heces de las personas con COVID-19, según los CDC, hasta la fecha no hay información de que nadie haya enfermado de COVID-19 debido a la exposición directa a aguas residuales tratadas o no tratadas
Más información de los CDC, aquí
¿Quién debe hacerse la prueba?
(haga clic en cada casilla para ampliar los detalles)
Si tiene síntomas de COVID-19 o si estuvo en contacto cercano con alguien con COVID-19, debe hacerse la prueba independientemente de su estado de vacunación.
Los síntomas notificados por personas con COVID-19 varían desde aquellos que presentan síntomas leves hasta quienes se enferman gravemente. Los síntomas pueden aparecer de 2 a 14 días después de la exposición al virus. Cualquiera puede tener síntomas de leves a graves. Las personas con estos síntomas podrían tener COVID-19:
- Fiebre o escalofríos
- Tos
- Dificultad para respirar (sentir que le falta el aire)
- Fatiga
- Dolores musculares y corporales
- Dolor de cabeza
- Pérdida reciente del olfato o el gusto
- Dolor de garganta
- Congestión o moqueo
- Náuseas o vómitos
- Diarrea
Esta lista no incluye todos los síntomas posibles. Los CDC seguirán actualizando esta lista a medida que aprendamos más acerca del COVID-19. Los adultos mayores y las personas con afecciones subyacentes graves, como enfermedades cardiacas o pulmonares o diabetes, parecen correr mayor riesgo de presentar complicaciones más graves a causa del COVID-19.
Cuándo buscar atención médica de emergencia
Esté atento a los signos de advertencia de emergencia* del COVID-19. Si alguien presenta alguno de estos signos, busque atención médica de emergencia de inmediato:
- Dificultad para respirar
- Dolor o presión persistente en el pecho
- Confusión
- Incapacidad de despertarse o permanecer despierto
- Piel, labios o lechos de uñas pálidos, grises o azulados, según el tono de la piel
*Esta lista no incluye todos los síntomas posibles. Llame a su proveedor de servicios médicos por cualquier otro síntoma grave o que le preocupe.
Llame al 911 o llame antes a su centro de emergencias local: notifique al operador que necesita atención para alguien que tiene o podría tener COVID-19.
Si ha estado en contacto directo con alguien con COVID-19, debe hacerse la prueba independientemente de su estado de vacunación. El contacto estrecho significa estar a menos de 6 pies de alguien durante 15 minutos o más en el transcurso de un día, con o sin una máscara o una cubierta para la cara.
Si se somete a la prueba porque ha estado en contacto estrecho con alguien que tiene COVID-19, es mejor que espere tres días después de haber estado juntos antes de hacerse la prueba. La prueba es menos precisa si te haces la prueba demasiado pronto. Debes permanecer en casa y alejado de los demás mientras esperas.
¿Qué hacer después de un resultado positivo?
Le rogamos que comunique cualquier resultado positivo de la prueba lo antes posible a través de este enlace de la encuesta, para iniciar el proceso de investigación y apoyo del caso. ¿Necesita ayuda? Llame al 866-917-8881
(haga clic en cada casilla para ampliar los detalles)
Le rogamos que comunique cualquier resultado positivo de la prueba lo antes posible a través de este enlace de la encuesta, para iniciar el proceso de investigación y apoyo del caso. ¿Necesita ayuda? Llame al 866-917-8881
El aislamiento se utiliza para separar a las personas infectadas por el COVID-19 de aquellas que no están infectadas.
Las personas en aislamiento deben quedarse en sus casas hasta que sea seguro estar en contacto con otras personas. En casa, quienes están enfermos o infectados deben separarse de las demás personas, permanecer en un área o “habitación para enfermos” específicas, y usar otro baño (si está disponible).
Cuánto tiempo hay que aislar – Público en general
Aislamiento: las personas (incluidos los entornos K-12) que hayan dado positivo en la prueba de COVID-19 sin síntomas o que muestren síntomas leves o moderados de COVID-19 deben aislarse independientemente del estado de vacunación.
Inicie el aislamiento durante 5 días completos.
Las personas pueden terminar el aislamiento después de 5 días completos desde el inicio de los síntomas si no tienen fiebre durante 24 horas sin usar medicamentos antifebriles y sus otros síntomas han mejorado.
El día 0 es el día en que comenzaron los síntomas o el día en que la persona se sometió a una prueba con resultado positivo. El día 1 es el día siguiente al inicio de los síntomas o, si la persona no tiene síntomas, el día siguiente a la realización de la prueba con resultado positivo (utilice la fecha de recogida de la prueba).
Si la persona sigue teniendo fiebre o sus otros síntomas no han mejorado después de 5 días de aislamiento, debe permanecer aislada hasta que no tenga fiebre durante 24 horas sin usar medicamentos antifebriles y sus otros síntomas hayan mejorado.
Las personas deben seguir llevando una mascarilla bien ajustada alrededor de otras personas en casa y en lugares públicos durante otros 5 días (del día 6 al día 10) después del final de su aislamiento de 5 días.
Las personas, independientemente de su estado de vacunación, con enfermedad grave o crítica, incluidas las que fueron hospitalizadas por su enfermedad COVID-19, o que están gravemente inmunodeprimidas, el periodo mínimo de aislamiento es de 20 días. Es decir, estos casos deben aislarse hasta que hayan transcurrido al menos 20 días desde el inicio de los síntomas o hasta que la primera prueba sea positiva, lo que ocurra antes, y que no hayan tenido fiebre sin utilizar medicamentos antifebriles y que los demás síntomas se hayan resuelto durante al menos 24 horas.
Sujeto a cambios. Para más detalles, visite la página web del Centro de Control y Prevención de Enfermedades sobre cuarentena y aislamiento.
Qué hacer
- Monitoree sus síntomas. Si tiene algún signo de advertencia de emergencia (como dificultad para respirar), busque atención médica de emergencia de inmediato.
- Permanezca en una habitación separada del resto de los miembros del hogar, si es posible.
- Use un baño separado, si es posible.
- Evite tener contacto con otros miembros del hogar y con las mascotas.
- No comparta los artículos del hogar de uso personal como tazas, toallas y utensilios.
- Use mascarilla al estar con otras personas si puede hacerlo.
Obtenga más información sobre qué hacer si se siente enfermo y cómo notificar a sus contactos.
Utilice la herramienta de cálculo de cuarentena y aislamiento de los CDC para ayudar a determinar cuánto tiempo necesita aislar, poner en cuarentena o tomar otras medidas para evitar la propagación de COVID-19.
Le rogamos que comunique cualquier resultado positivo de la prueba lo antes posible a través de este enlace de la encuesta, para iniciar el proceso de investigación y apoyo del caso. ¿Necesita ayuda? Llame al 866-917-8881
El aislamiento se utiliza para separar a las personas infectadas por el COVID-19 de aquellas que no están infectadas.
Las personas en aislamiento deben quedarse en sus casas hasta que sea seguro estar en contacto con otras personas. En casa, quienes están enfermos o infectados deben separarse de las demás personas, permanecer en un área o “habitación para enfermos” específicas, y usar otro baño (si está disponible).
How Long to Isolate – General Public
Isolation: people (not in K-12 or healthcare settings) who have tested positive for COVID-19 with no symptoms or are showing mild to moderate symptoms of COVID-19 should isolate regardless of vaccination status.
- Start isolation for 5 full days.
- Individuals can end isolation after 5 full days since symptom onset if they are fever-free for 24 hours without the use of fever-reducing medication and their other symptoms have improved.
- Day 0 is the day symptoms began or the day the person took a test that had a positive result. Day 1 is the day after symptoms began or, if a person does not have symptoms, the day after the person tested positive (use the date the test was collected).
- If they continue to have fever or their other symptoms have not improved after 5 days of isolation, they should stay in isolation until they are fever-free for 24 hours without the use of fever-reducing medication and their other symptoms have improved.
- Individuals should continue to wear a well-fitting mask around others at home and in public places for an additional 5 days (day 6 through day 10) after the end of their 5-day isolation.
People regardless of vaccination status with severe to critical illness, including those who were hospitalized for their COVID-19 illness, or who are severely immunocompromised, the minimum period of isolation is 20 days. That is, these cases should isolate until at least 20 days since symptom onset or first positive test, whichever is earlier, and they have been fever free without the use of fever-reducing medications with other symptoms resolving for at least 24 hours.
Subject to change. For further details visit the Center for Disease Control and Prevention Quarantine and Isolation webpage.
Qué hacer
- Monitoree sus síntomas. Si tiene algún signo de advertencia de emergencia (como dificultad para respirar), busque atención médica de emergencia de inmediato.
- Permanezca en una habitación separada del resto de los miembros del hogar, si es posible.
- Use un baño separado, si es posible.
- Evite tener contacto con otros miembros del hogar y con las mascotas.
- No comparta los artículos del hogar de uso personal como tazas, toallas y utensilios.
- Use mascarilla al estar con otras personas si puede hacerlo.
Obtenga más información sobre qué hacer si se siente enfermo y cómo notificar a sus contactos.
¿Qué hacer después de una exposición a COVID-19/ contacto cercano?
(haga clic en cada casilla para ampliar los detalles)
La cuarentena se utiliza para separar y restringir el movimiento de las personas que estuvieron expuestas a una enfermedad contagiosa para ver si se enferman después de un contacto cercano (a menos de 6 pies de distancia de alguien durante un total acumulado de 15 minutos o más en un período de 24 horas) con alguien que tiene COVID-19.
A partir del 12 de marzo, ya no se recomendará la cuarentena para las personas de la población general que hayan estado expuestas a alguien que tenga COVID-19, independientemente del estado de vacunación. Esto incluye a los niños y al personal de los centros de enseñanza primaria y secundaria y de las guarderías.
Se recomienda que:
- Considerar el uso de una máscara bien ajustada durante 10 días después de la exposición.
- Estar atentos a los síntomas hasta 10 días después de la exposición.
- Si tiene síntomas, autoaislarse inmediatamente y ponerse en contacto con las autoridades locales de salud pública o con su proveedor de atención médica.
Información de los CDC, ver más aquí.
Utilice la herramienta de cálculo de cuarentena y aislamiento de los CDC para ayudar a determinar cuánto tiempo necesita aislar, poner en cuarentena o tomar otras medidas para evitar la propagación de COVID-19.
La cuarentena se utiliza para separar y restringir el movimiento de las personas que estuvieron expuestas a una enfermedad contagiosa para ver si se enferman después de un contacto cercano (a menos de 6 pies de distancia de alguien durante un total acumulado de 15 minutos o más en un período de 24 horas) con alguien que tiene COVID-19.
How Long to Quarantine – General Public
Quarantine: People (excludes those in K-12 or healthcare settings) who come into close contact with someone with COVID-19 quarantine length depends upon vaccination status.
Those up to date on COVID-19 vaccination as defined by CDC (see definition below) AND individuals who had confirmed COVID-19 (tested positive using a COVID-19 viral test) within the last 90 days:
- No quarantine required.
- Wear a well-fitting mask around others for 10 days from the date of their last close contact with someone with COVID-19 (the date of last close contact is considered day 0) and watch for symptoms of COVID-19.
- Recommended to get tested at least 5 days after having close contact with someone with COVID-19. If they test positive or develop COVID-19 symptoms, they should follow recommendations for isolation.
Those NOT up to date on COVID-19 vaccination as defined by CDC (see definition below):
- Quarantine for at least 5 days after their last close contact with someone with COVID-19. Day 0 is the last day you had close contact with the infected individual.
- Individuals in quarantine should not go to work or other in-person events/activities during their quarantine period.
- Wear a well-fitting mask around others for 10 days from the date of their last close contact with someone with COVID-19 (the date of last close contact is considered day 0) and watch for symptoms of COVID-19.
- Recommended to get tested at least 5 days after having close contact with someone with COVID-19. If they test positive or develop COVID-19 symptoms, they should follow recommendations for isolation.
- If unable to wear a mask, an individual should complete a 10-day quarantine.
- If an individual is unable to quarantine, they should wear a well-fitting mask around others at home and in public for 10 days.
Subject to change. For further details visit the Center for Disease Control and Prevention Quarantine and Isolation webpage.
vaccination status Up to Date definition:
-
Boosted,
-
or completed the primary series of Pfizer or Moderna within the last 6 months,
-
or completed the primary series of J&J within the last 2 months.
vaccination status NOT Up to Date definition:
-
unvaccinated,
-
or has not completed the primary series of any COVID-19 vaccine,
-
or completed the primary series of Pfizer or Moderna over 6 months ago and is not boosted,
-
or completed the primary series of J&J over 2 months ago and is not boosted.
Qué hacer
- Quédese en casa por 14 días después de su último contacto con una persona que tiene COVID-19.
- Esté atento a la aparición de fiebre (100.4 ºF), tos, dificultad para respirar u otros síntomas del COVID-19.
- Si es posible, manténgase alejado de las personas que viven con usted, en especial de aquellas con mayor riesgo de enfermarse gravemente a causa del COVID-19.
Después de la cuarentena
- Estar atento a los síntomas hasta 14 días después de la exposición.
- Si tiene síntomas, debería aislarse de inmediato por cuenta propia y notificar a la autoridad de salud pública local o a su proveedor de atención médica.
Información de los CDC, ver más aquí.
Utilice la herramienta de cálculo de cuarentena y aislamiento de los CDC para ayudar a determinar cuánto tiempo necesita aislar, poner en cuarentena o tomar otras medidas para evitar la propagación de COVID-19.
Tratamiento y recursos comunitarios
(haga clic en cada casilla para ampliar los detalles)
Ahora hay más opciones de tratamiento disponibles en la lucha contra la enfermedad por coronavirus. Hable con su proveedor de atención médica sobre las opciones de tratamiento disponibles si tiene COVID-19 tan pronto como sea posible, algunas opciones de tratamiento deben iniciarse tan pronto como 5 días después de la fecha de la prueba positiva.
Su proveedor sabrá cuál es la mejor opción para usted, basándose en sus síntomas, riesgos e historial de salud.
¿Qué tratamientos existen para la COVID-19?
La mejor manera de combatir el COVID-19 es evitar que se contagie. Eso significa llevar una mascarilla bien ajustada, mantener las reuniones reducidas y al aire libre si es posible y vacunarse (incluyendo una dosis de refuerzo si es posible).
Pero el virus sigue propagándose ampliamente, por lo que incluso si sigue todos los protocolos de seguridad puede infectarse, y potencialmente enfermar gravemente.

Aunque la mayoría de los casos de COVID-19 no requieren hospitalización, algunas personas tienen afecciones que aumentan el riesgo de infección grave, como el asma, la diabetes o las enfermedades cardíacas. También pueden estar tomando medicamentos que debiliten su sistema inmunológico o tener una enfermedad crónica que pueda empeorar los efectos de la COVID-19. Los CDC tienen una lista completa de ciertas condiciones médicas que hacen que alguien tenga un mayor riesgo.
Para estas personas, hay varios tratamientos de COVID-19 disponibles:
Tratamientos antivirales orales de Pfizer, Merck
La FDA ha aprobado recientemente dos medicamentos antivirales orales que reducen drásticamente las posibilidades de hospitalización, pero deben administrarse lo antes posible después de un diagnóstico positivo de COVID-19 y dentro de los primeros cinco días de los síntomas para que sean eficaces.
- Paxlovid (de Pfizer) actúa interrumpiendo la capacidad de mutación del virus. Se dirige específicamente a una enzima que ayuda a que ciertas proteínas víricas se formen correctamente.
- El molnupiravir (de Merck) actúa introduciendo mutaciones directamente en la composición genética del virus. Cuando el virus se copia a sí mismo, muta tanto que ya no puede funcionar. Hay algunas preocupaciones de seguridad porque altera la información genética del virus. Algunos expertos se preocupan por los efectos adversos, especialmente en las personas embarazadas y en los niños.
Debido a la escasez nacional, ninguno de estos medicamentos está ampliamente disponible. No vaya a la sala de emergencias en busca de estos medicamentos si no requiere atención de emergencia. Si tiene síntomas, consulte a su médico habitual si lo tiene, o visite una clínica de atención urgente o llame a la farmacia adventista al 503-815-2341 para hablar con un farmacéutico.
Considere la posibilidad de establecer atención con un proveedor utilizando los siguientes contactos: Tillamook County Community Health Center (503-842-3900), Adventist Health Tillamook (503-842-5546) o Rinehart Clinic (1-800-368-5182).
Remdesivir
El medicamento antiviral remdesivir también actúa sobre el material genético del virus, bloqueando su capacidad de mutar. El remdesivir (también conocido por su nombre comercial, Veklury) fue aprobado por primera vez en octubre de 2020 para los pacientes de COVID-19 de 12 años o más que requieran hospitalización. El 21 de enero de 2022, la FDA modificó su aprobación para incluir a los pacientes de COVID-19 de 12 años o más que no requieren hospitalización pero que tienen riesgo de padecer una enfermedad grave. Además, la FDA ha autorizado el remdesivir para pacientes pediátricos menores de 12 años que pesen al menos 3,5 kg (unas 7 libras).
Anticuerpos monoclonales
Los anticuerpos monoclonales actúan imitando una de las respuestas inmunitarias del organismo. Cuando el sistema inmunitario detecta un invasor extraño, como un virus, libera anticuerpos. Estos anticuerpos se adhieren al virus y le indican al sistema inmunitario qué células debe destruir.
Los anticuerpos monoclonales se crean en un laboratorio y se administran mediante una inyección directamente en el torrente sanguíneo, o en un brazo u otra zona del cuerpo, como una inyección.
Existen varios tratamientos con anticuerpos monoclonales actualmente autorizados en EE.UU., y cada uno de ellos funciona de forma ligeramente diferente. Sin embargo, sólo uno, llamado Sotrovimabv, parece ser eficaz contra la variante Omicron.
Sólo algunas personas pueden recibir anticuerpos monoclonales. Consulte la tabla siguiente para conocer las pautas de elegibilidad.
(Gráfico de: https://combatcovid.hhs.gov/i-have-covid-19/how-do-i-know-if-im-high-risk y contenido de esta sección de https://covidblog.oregon.gov/what-kind-of-treatments-exist-for-covid-19/)
La FDA sigue trabajando con los desarrolladores, investigadores, fabricantes, los Institutos Nacionales de Salud y otros socios para ayudar a acelerar el desarrollo y la disponibilidad de medicamentos terapéuticos y productos biológicos para prevenir o tratar la COVID-19. Para comprobar si un medicamento está aprobado por la FDA, busque en la base de datos de medicamentos aprobados visitando la base de datos Drugs@FDA.
¿Qué debo hacer si tengo, o creo que tengo, COVID-19?
Los Centros para el Control y la Prevención de Enfermedades tienen recomendaciones para las personas que están enfermas de COVID-19 o que creen que pueden tener COVID-19.
En general, la mayoría de las personas tienen una enfermedad leve y pueden recuperarse en casa. Si cree que ha estado expuesto a la COVID-19, notifique a su médico, controle sus síntomas y obtenga atención médica de urgencia inmediatamente en caso de signos de advertencia de emergencia, como problemas para respirar.
Si cree que tiene COVID-19 y necesita una prueba, póngase en contacto con su proveedor de atención médica, el departamento de salud local o llame al 211 para encontrar un sitio de pruebas en la comunidad.
Esta información procede del U.S. Food & Drug Administration page
¿Cómo puedo acceder a estos tratamientos?
Dependiendo de su historial médico, riesgos y síntomas, su proveedor de atención médica puede ayudarle a determinar si una terapia aprobada por la FDA, o disponible bajo una EUA, es adecuada para usted.
Los siguientes sitios web contienen información sobre el acceso a los tratamientos con anticuerpos monoclonales para la COVID-19:
Esta información procede del U.S. Food & Drug Administration page
¿Qué pasa si mi proveedor de atención médica no conoce estas opciones de tratamiento?
La información sobre las opciones de tratamiento está disponible en la página web de preguntas frecuentes sobre COVID-19.
Para obtener información específica sobre las EUA, dirija a su proveedor de atención médica a la página de Autorización de Uso de Emergencia (EUA) de la FDA, donde hay hojas informativas para los proveedores de atención médica sobre los tratamientos autorizados. Su proveedor de atención médica también puede ponerse en contacto con nuestra División de Información sobre Medicamentos en el 301-796-3400 o en druginfo@fda.hhs.gov.
Esta información procede del U.S. Food & Drug Administration page
Permanecer en casa hasta que no pueda propagar el virus es importante, pero quedarse en casa puede no ser fácil. Si necesita ayuda, hay opciones para apoyarle.
Si necesita ayuda para encontrar un lugar de aislamiento o cuarentena, llame al Centro de Salud Comunitaria del Condado de Tillamook al 503-842-3924.
Si necesita ayuda con la entrega de alimentos, comestibles o medicamentos, llame a la línea de atención de la YMCA al: 503-374-0750.
Si desea hablar con alguien sobre las emociones difíciles que puede estar sintiendo, sepa que no está solo. Hay profesionales formados que esperan su llamada o su mensaje:
-
- Tillamook Family Counseling Center: (503) 842-8201 or 1-800-962-2851.
- Tides of Change: 503-842-9486
- National Suicide Prevention Lifeline – 800-273 TALK(8255); www.suicidepreventionlifeline.org
- Oregon Senior Peer Outreach: 1800-736-4676
- SAMHSA Disaster Distress Hotline: 1800-985-5990
- Senior Loneliness Line: 503- 200-1633
- The Friendship Line – 1800-971-001
- Dual Diagnosis Anonymous: online meeting schedule
- Helping Children Cope – online resource
- National Alliance for Mentally Ill (NAMI)- www.namiwash.org
Definiciones
(haga clic en cada casilla para ampliar los detalles)
- Boosted,
- or completed the primary series of Pfizer or
Moderna within the last 6 months, - or completed the primary series of J&J within
the last 2 months.
- Unvaccinated,
- or has not completed the primary series of any COVID-19 vaccine
- or completed the primary series of Pfizer or Moderna over 6 months ago and is not boosted,
- or completed the primary series of J&J over 2 months ago and is not boosted.
Presentamos nuestra nueva clínica de cuidados agudos COVID-19
Las pruebas y la atención de COVID-19 están disponibles para las personas que experimentan síntomas o que han tenido contacto cercano con un caso confirmado de COVID-19 en nuestra clínica de cuidados intensivos ubicada en 2111 8th St. Tillamook
Horas:.
De lunes a viernes
8:oo a.M.. A 12:00 p.M.